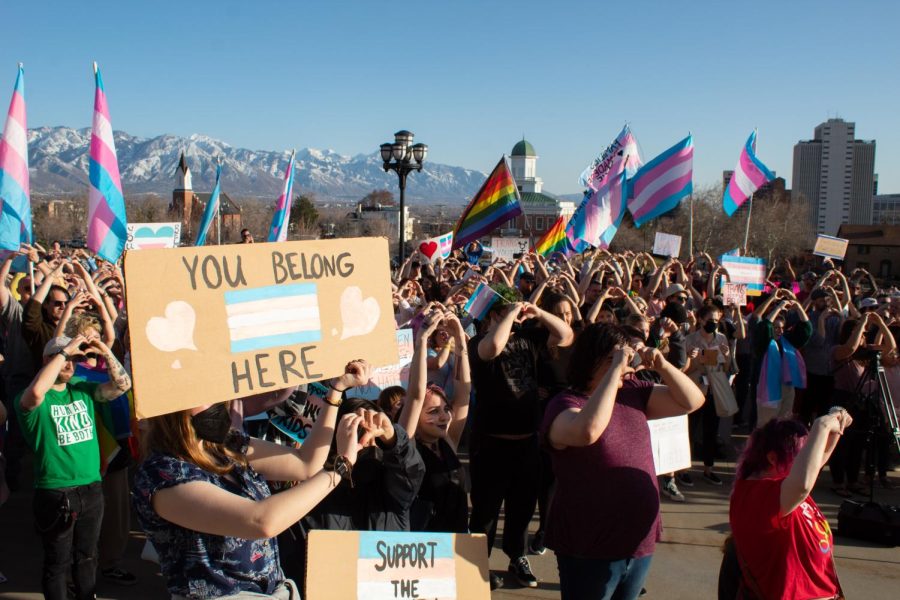Expanding Access to Gender-Affirming Care in Utah
Protestors hold hearts towards transgender youth sitting on the steps of the Utah State Capitol on March 24, 2022. (Photo by Carlene Coombs | The Daily Utah Chronicle)
November 16, 2022
In the 2023 Utah Legislative Session, lawmakers will hear a bill proposing to ban gender-affirming surgeries on minors. Similar legislation did not reach a committee vote in the 2022 session.
Erika Sullivan, an assistant professor of clinical family medicine and medical co-director of the University of Utah’s Transgender Health Program, does not speak on behalf of the U or the Transgender Health Program. She said this legislation is harmful and not based in science.
“The science shows that when people are offered gender-affirming care, they have better outcomes,” she said.
In an email statement not representing the U, Ariel Lee Malan, the outreach network and development specialist with the U’s Transgender Health Program, said gender-affirming care is age-appropriate, medically necessary, supported by all major medical organizations, well-researched and safe.
“Studies have shown us that transgender youth with access to gender-affirming care have lower rates of depression and suicidality,” Malan said.
Sullivan said those who seek this care are not deciding overnight.
“They have often known this about themselves for years and years and years, and making the decision to seek treatment for it — it’s not something that they take lightly,” she said. “They are making informed decisions that again, are informed by science and any legislation that limits that care, I think, is not medically sound.”
Gender-Affirming Care in Rural Areas
According to a 2019 report by the Movement Advancement Project, from 2014-17, roughly 16% of transgender people in the United States lived in rural areas — but research has shown there is a lack of gender-affirming care in these regions. One study found that 70% of transgender and gender diverse individuals in rural Appalachian areas would have to travel out of state to access gender-affirming care.
However, less is known about care for transgender individuals in the rural parts of Utah.
The U’s Transgender Health Program recognizes that more can be done to support transgender individuals across the state, so they offer some free continuing medical education courses and resources for interested providers to learn more about this care.
“I actually think there are quite a few providers in Utah who are offering this care, but we’re just not aware of it because they’re offering it and so those patients aren’t coming to see us,” Sullivan said.
When a patient interested in transitioning to the gender they identify with comes to Whitney Mack, a family doctor in Moab, Utah, together they discuss the implications, medication options and referrals. If someone is interested in surgery, for example, they are referred to the U because it is a specialized service.
“I’ll see everyone for anything, and then I transfer them to a specialist if the care gets out of my ability, but usually, no matter what the condition, whether it’s transgender health or stomach issues or mental illness, we can get started here with the treatment plan and testing if needed,” she said.
Mack can also help with lab work, and support someone in continuing their already established gender-affirming care.
“I think it’s provider-specific, meaning I am fairly comfortable providing this care,” she said. “I don’t know that everyone is, anywhere that people would go, no matter if they were in a city or out in rural areas.”
Expanding Care
Sullivan said gender-affirming care in Utah is important because “everyone should have equal access to healthcare.”
“The expectation should be that the providers that they see are knowledgeable about the medical questions that they have,” she said.
As a primary care physician, she acknowledged not everyone can be knowledgeable of every aspect of health — but she said evidence-based competence of care for transgender patients is “well within the purview of all primary care providers.”
Rather than a moral or religious objection, Sullivan thinks most providers don’t offer this care because they feel they were not trained on it.
“And they’re absolutely right,” she said. “They haven’t been trained on it. Gender-affirming care really is not taught in medical school, and only recently has it begun to be taught in residency programs and not uniformly at all in residency programs.”
Sullivan has made it her mission to expand the capacity of the healthcare workforce to more adequately provide care for the transgender population of Utah and surrounding states.
Usually, if providers are trained on gender-affirming care, they are trained during their residency years. Sullivan believes training should start in the pre-clinical years and then be expanded upon in residency programs. According to her, most providers offering these services in the primary care setting have not had additional fellowship training after residency.
“They probably either learn on the job just by seeing these patients and learning over time,” she said. “Or they said, ‘This is a community I want to serve, I need to seek out educational opportunities from a place that is doing continuing medical education.’”
There are some fellowship programs in other places, such as Los Angeles and Wisconsin, that allow people to specialize in LGBTQ+ care after their residency.
Mack learned how to provide this care in residency but she said “it was still pretty limited.” She added that her knowledge can always grow, so she researches and looks through different medical journals that offer advice on this type of care.
“But I also think that about everything, because we take care of so many medical conditions and such a broad amount of medical conditions that I’m always looking things up,” she said.
When Sullivan was in her residency program, they did not offer any formal teaching, so she learned on the job as a third-year resident. Along with Bernadette Kiraly, a family physician at the Sugar House Health Center Family Medicine Clinic at the U, Sullivan decided to change that — now, residents at the U receive training about offering these services.
“The residents do graduate with the necessary skills to be able to offer these services so we’ve changed, you know, what that looks like locally within our programs,” Sullivan said.
She said transgender care is a multidisciplinary field.
“And so it’s not enough to just say, ‘Oh, well, we’ll have primary care providers who can do hormone [therapy] and that’s all that transgender people need,'” she said. “That’s actually just the tip of the iceberg.”
According to Sullivan, there are a variety of people who need to get this training.
“We need surgeons who are familiar with offering these surgeries, we need urologists who are familiar with offering surgeries, we need speech therapists and mental health workers and counselors, pelvic floor physical therapists, obstetricians and gynecologists, people in reproductive endocrinology and adolescent medicine,” she said.
Mack said providing gender-affirming care is important, yet underrepresented as a service.
“All of the care that I provide tries to respect patient autonomy and give them control and just support what they want out of their own healthcare,” Mack said.
For those who haven’t been trained in medical school or residency, Sullivan recommended a continuing medical education program, although noting more work can be done to make these more affordable.
The U’s Transgender Health Program puts on a Transforming Care Conference every year for providers to learn more about how to offer this care.